Addressing trypanophobia to improve immunization & community health.
1. Tell the provider your plan (e.g. “I need to sit, I’m holding her hand, and don’t tell me when you do it.”)
2. Control pain with science-proven interventions.
Studies showing what works for Adult injections: Buzzy:4 EMLA:1 Cold:2 Fake Cough: 1
Studies showing what works for kids: Buzzy 18 Shotblocker 1(insulin only) swearing: 1
3. Fainter? Drink a pint 1 hour before, tense stomach during. Use Buzzy during procedure.
4. Distraction During: Count something!
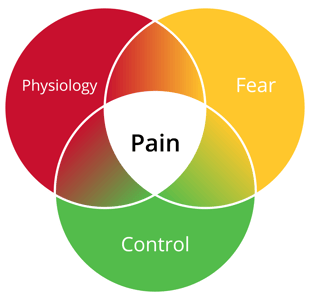
The amount of physiological pain, fear, and sense of control in a procedure is what the brain perceives as distress. Address all three elements for a better needle experience.
It’s not just ANY topical anesthetic cream – only EMLA (lidocaine + prilocaine) has been studied for immunizations,(6) with almost all studies in the infant age range. While the creams may have similar efficacy for drawing labs, vaccines hurt more: the studies should be considered separately. Prescription EMLA not only penetrates more deeply than LMX,(7) the effect lasts up to 4 hours, while 4% lidocaine wears off. For pain relief, EMLA must be on at least 60 minutes. There is only one single immunization study in the 4-6 year range using EMLA compared to placebo, and it found 61% pain reduction.(8) A Danish study in 12 year olds found no difference. The infant data should contribute some strength, but in the 4-6 year range the application of creams for an hour can raise anxiety which increases pain.
Ice on the spot can help older kids, but sprays get too cold even for adults. In the 4-6 year range, one researcher found cold spray worked as well as a placebo spray (1995), one didn’t,(9) and two other studies also used distraction to address fear and focus, blurring results from spray.(10) Buzzy outperformed cold spray for IVs, with a 3x better success on the first stick.(24)
Mechanical stimulation in the 200Hz frequency works for lab draws. Since vaccines hurt more, in kids vibration alone did not help(2 – 7 years)(11) For adults, adding 1 minute of M-stim vibration before and after an injection could reduce arm pain, and vibration alone reduces pain. More importantly, Buzzy works best for adults who were anxious about needles. (Redfern et al).

Cold and vibration reduced pain 70% in 41 4-6 year olds;(12) simultaneous vibration + cold (Buzzy) reduced injection pain 40% in 50 3 – 18 year olds;(13) another study found Buzzy reduced pain 74% in 104 7 year olds receiving a TDaP;(14) and several other studies also show pain reduction for adult flu immunization,(15) Diclofenac by 74% for adults,(16) and Bicillin by 50%.(17)
To help an adult friend control panic to get protected, matter-of-fact empathy helps most. Be prepared to intervene if a caregiver is dismissive, distract while waiting, and help them with their plan, whether hand-holding, having a TikTok to show, or coaching deep breaths.
Pain, expected pain, and fear are highly correlated.(2, 3) Addressing both pain and fear is synergistic for relief – more than the sum of its parts.(4, 5) To prevent or treat most needle anxiety, addressing both pain and fear while changing the focus during a procedure is the best practice.
The most groundbreaking new work here is the degree to which parents influence their young child’s fear. Campbell and Pillai at York University have followed preschool children’s behaviors during vaccines since birth, and found that “caregiver behaviors during vaccinations are … critical to both child pain coping responses and outcomes in the short- and long-term.”(18) For older kids, multiple studies and two meta-analyses show that Buzzy reduces injection anxiety.(19) To best control fear, though, since post-traumatic stress is heavily influenced by parent’s signals,(20) parents need to get a grip. Tips: be warm but no-nonsense, and praise the child’s effort at coping while reinforcing that vaccines keep them safe..
Needle phobia, trypanophobia, “Blood injection injury phobia”, and balanophobia all can cause an extreme fear of medical procedures involving injections or needles. For most people who have this fear, it develops around age 4 or 5 with a bad immunization experience.
Additionally, about 3-5% of women and 1-2% of men have a genetic predisposition to getting light-headed or fainting (ie vasovagal syncope) in response to needle procedures. While this can lead to an avoidance or fear of needles, it starts out as physiologic response first.
In 1995, the incidence of adult needle phobia ranked at 10%. A study in 2012 found a that numbers had risen to 24%.
Similarly, a 2012 survey by Target found 23% of those who didn’t get a flu shot avoided it because of the needle.
For children, the incidence changed from 25% in 1995 to 63% in 2012 — 252% increase in less than 2 decades.
Needle phobia can have some disturbing side effects. Our NIH research showed children with high needle fear were 2.5x less likely to complete their HPV series than those with low fear. Fear of needles is a barrier to health.
Needle phobia affects personal and public health in profound ways.
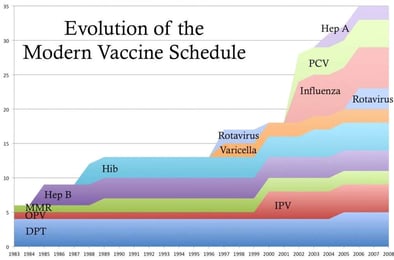
Protecting anyone from life-long needle phobia must start from their first memorable experiences with needles. Even with children who are pre-disposed to fainting, other factors play an important role in the development of a health-threatening phobia.
If parents and professionals intervene early on in children’s lives, it can help protect them from developing this health-threatening condition. The more vaccines we give in early childhood, the more opportunities for traumatic memory and association with doctors. As we add more vaccines, we MUST add protective ways of decreasing the negative reaction to healthcare.
Distraction mediates both fear and pain in needle procedures. Numerous studies show the effectiveness of distraction in reducing pain and negative emotions during injections.
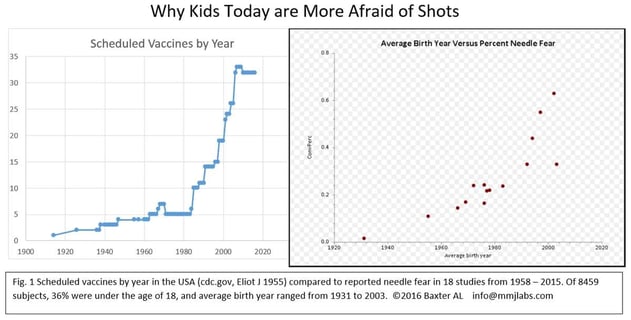
Needle pain management is one of the most effective interventions. During the first encounters with needles, needle pain management and distraction can protect the child from traumatic experience associated with medical procedures and the clinical environment and experience, and prevent the child from developing anxiety and even phobia later in her life.
The best interventions deal with both pain directly as well as fear and focus. Learning to distract oneself from pain is a lifelong coping strategy.
Physical ways to reduce IV pain include Buzzy®, topical anesthetics, and alternative injection methods like J-Tip. For injections, Buzzy is the most studied and effective, and the only intervention that reduces fear. For a breakdown of these methods for adults, Dr. Baxter testified to HHS Vaccine Advisory Committee in 2021.
According to clinical research, Buzzy® Pain Relief can reduce IV needle pain by 80%; some studies have looked at both pain and fear. Used with DistrACTION® Cards, Buzzy® can almost completely eliminate pain (down to 0.53 on a 10 point scale, Inal S.). The physiology of cold and vibration, called Gate Control, naturally blocks out the competing stimulation of pain. Controlling as many aspects of a medical visit as possible is one way to control your fear of needles.
As a byproduct of developing Buzzy, Dr. Baxter discovered the abrupt rise in needle fear, and constructed the multimodal model of pain/fear/focus reduction to comprehensively address the problem. In addition to TEDx and TEDMED talks about the causes and consequences of needle phobia, Dr. Baxter presents research on the subject and writes scholarly articles. Contact us directly if you are interested in the subject, have a solution to share, or plan a research study.
Dr. Anna Taddio and her group in Canada do a marvelous job of creating guidelines for improving vaccination pain(1) every 5 years. Previously the research was based on IV access studies. It is now known that injections are approximately twice as painful as IV, so a different research base is being used. Buzzy has the most injection proof of any intervention. For children, breathing with a toy or bubbles, verbal video, and music distraction have weak research support. As of 2021, here is the most current data on reducing vaccine pain and fear for the 4+ age range. These children are old enough to remember, so reducing medical trauma matters to their future independent uptake of healthcare. Many of these techniques are applicable to adults, too.
"Buzzy has literally changed my life. Needle phobia GONE."
Angela Vermillion
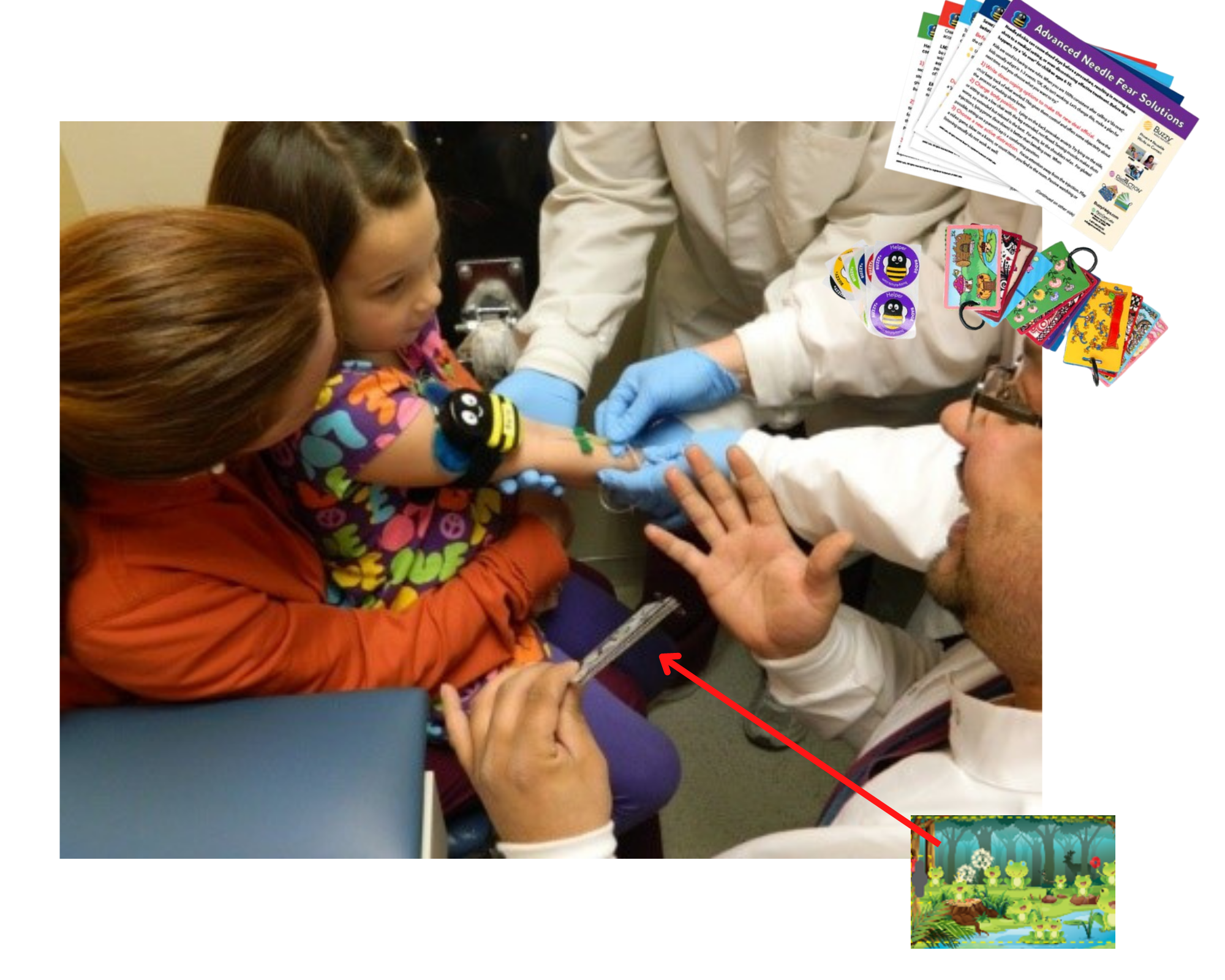
While a few studies incorporate blowing bubbles as distractions for lab draws, quality fear data for immunizations is scant. In multiple studies, DistrACTION cards (visual cards requiring a task) reduced venipuncture anxiety more than blowing a balloon, kaleidoscopes, or watching a video.(21) Compared to nothing, 97% reported a better experience than previous with DistrACTION cards, but this was for 7-10 year olds undergoing venipuncture.(22)
Overall, the most current review of immunization pain and anxiety reduction concluded, “Interventions using coolant and vibration together, as well as a combination of site-specific and patient-led interventions, showed the most consistent effects in reducing self-reported pain, fear or distress.”(23)
We do know that active distraction is better than passive, but there currently is not evidence to recommend bubbles over DistrACTION cards or Virtual Reality – probably iPad research will end up being the best. We really need to know.
For adults already afraid, using a pain reliever reduces fear by half after three experiences. Adding distraction probably helps more, or faster, but hasn’t been studied. Tips for teens actually often work well for adults.

Amy Baxter MD has been a fellow of the American Academy of Pediatrics and the American College of Emergency Physicians, and is a Clinical Associate Professor of Emergency Medicine at the Medical College of Georgia Augusta University. Since 2016 she has been the full time CEO of Pain Care Labs, making external neuromodulatory over the counter pain relief devices Buzzy and VibraCool. She has advocated for humane vaccination with ZDoggMD, at TEDx and discussed her research at TEDMED talks, among others. To date, Buzzy has been used to block pain from over 37 million needle procedures.
Find out how DistrACTION® cards can be used to further reduce pain and anxiety.